Cholesterol & Lipids Overview
Cholesterol is an essential component for life and health.
But why do we care about cholesterol levels in the first place? What difference does it make?
We care because cholesterol patterns may indicate higher risk for cardiovascular disease. Our goal is to decrease the risk of cardiovascular disease.
However, cholesterol is not now, nor has it ever been, the issue!
You may have had your “cholesterol” checked as part of a wellness exam. The reality is that you have had your lipoproteins checked.
Total Cholesterol (TC) – this is the total cholesterol measured on a cholesterol or lipid panel. Mainstream medical recommendations are that TC is <200. However, total cholesterol is not a risk factor for disease. Don’t be concerned about this value!
Triglycerides (TG) – also known as triacylglycerol. These are 3 fatty acids attached to a glycerol backbone. This is how fats are transported in the blood. Recall that blood is largely composed of water. Water & oil (fat) don’t mix. Lipoproteins enable transportation of TGs in the watery environment of blood and carry them to their destination. The goal for TG is certainly <200 but we would like <150. I argue that it is actually an indicator of other problems that increase risk and doesn’t increase risk in and of itself.
Understand that when we are checking your “cholesterol” we are not really checking your cholesterol. We are actually measuring your lipoproteins. Fats and cholesterol do not mix with water (blood) and have to be carried in a lipoprotein molecule. We classify these lipoprotein particles based on their composition. The largest of these are the chylomicrons followed by very low-density lipoproteins, LDL, and then HDL. The density was originally defined by ultracentrifugation and is determined by the composition of the molecule. The composition of each of these molecules is determined by the proteins (apolipoproteins) on the membrane of the molecule.
Chylomicrons
Chylomicrons are composed primarily of triglycerides (85%) but also contain 3% cholesterol esters, 2% cholesterol, and 8% phospholipids. They are the primary transporters of fats after fatty meals.
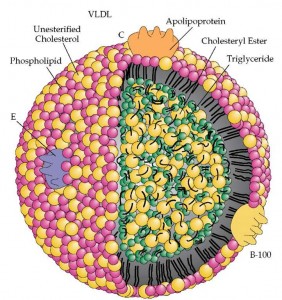
Very Low-Density Lipoproteins (VLDL)
 Low-Density Lipoproteins (LDL)
Low-Density Lipoproteins (LDL)
LDL is traditionally referred to as the ‘bad’ cholesterol. It is called ‘low density’ because it is composed of a larger amount of TGs. The traditional goal for LDL for standard risk patients is 130 or less. However, small-dense LDL (sdLDL) may be a better indicator of risk of cardiovascular disease. LDL particle number may be the best indicator of cardiovascular disease risk. The goal is to decrease the risk of small, dense LDL particle. 2 things are responsible for increasing small, dense LDL particle: genetics (nothing you can do about that) and carbohydrates. If you want to decrease your risk of cardiovascular disease, decrease your carbohydrates! Read this article for more information.
High-Density Lipoproteins (HDL)
these are what has been referred to as the ‘good’ cholesterol. HDL seems to play an increasingly important role as an indicator of reducing cardiovascular risk. Normal values are typically between 35 and 70. HDL is anti-inflammatory and functions to pick up cholesterol from the peripheral tissues and transport it back to the liver (Reverse Cholesterol Transport – see below).
Non-HDL-c
Non-HDL-c is simply calculated from subtracting HDL from Total Cholesterol. It is everything except the HDL. Non-HDL-c is suggested to be better correlated with cardiovascular disease. In other words, it seems to be a better risk predictor.
Goal – < 130 mg/dL
What to do about it – improve overall health using the ‘Healthy Trinity’
Apo B
ApoB is the protein attached to the LDL molecule. It is the scientifically accepted measurement of atherogenic particle number. ApoB traverses in the blood in a 1:1 ratio with chylomicrons, VLDL, IDL, LDL and Lp(a). Several studies identified elevated ApoB concentrations to be highly predictive of cardiovascular events. Most studies have found ApoB to be a more reliable indicator of cardiovascular event risk than LDL-C.
Goal – < 60 mg/dL, < 55 mg/dL with CHD & CHD risk equivalents
What to do to improve it –
LDL-P
This is the actual number of particles of LDL measured in the sample. It is determined by NMR (Nuclear Magnetic Resonance). Studies have shown that elevated LDL particle concentration is associated with increased risk for coronary heart disease, even in the presence of optimal LDL cholesterol values.
Goal – < 1000 nmol/L
What to do to improve it – Focus on the ‘Healthy Trinity’
sdLDL-C
Small LDL particles may be observed in association with the metabolic syndrome and pre-diabetes. Statins, while they can lower the number of LDL particles, do not change the size of the LDL particles. sdLDL is commonly present in insulin resistant patients. The small size of LDL particles enhances endothelial penetration and accelerates atherosclerosis and lipoprotein oxidation. It is associated with a 3x increased risk of MI & stroke.
Goal – < 21 mg/dL
What to do to improve it – Focus on the ‘Healthy Trinity’ and specifically blood sugar control. We recommend Wheat Belly by Dr William Davis for more information on this topic. Smoking cessation, exercise, dietary restrictions, weight loss (as appropriate), and moderate alcohol intake can impact sdLDL as well.
% sdLDL-C
This is a percentage. It is how much small, dense LDL there is as a percentage of the total amount of LDL. It is mathematically derived.
Goal – < 13%
What to do to improve it – Do the same things stated above for sdLDL.
Apo A-1
ApoA-1 is the protein associated with the HDL molecule. It corresponds with the ApoB on the LDL molecule. Low levels suggest low cholesterol clearance. When ApoA1 is low there is a 3x increased risk of MI & stroke.
Goal – > 131 mg/dL
What to do to improve it – improve overall health & HDL
HDL-P
Total HDL particle decrease has been associated with increased risk for cardiovascular disease. HDL particle concentration may be increased with exercise, fish oil, niacin, fibric acids, or moderate consumption of alcohol.
Goal – > 35.0 μmol/L
What to do to improve it – as above
HDL2-C
HDL2 is the largest of the HDL molecules and is the one responsible for the majority of the Reverse Cholesterol Transport. It seems to indicate greater protection and may be a marker for plaque regression. It is thought to have anti-oxidant properties. When HDL2-C is low it suggests a 2-3x increased risk of CVD.
Goal – > 12 mg/dL
What to do to improve it – as above
Apo B: Apo A-1 Ratio (Calculated)
Recently large case control studies have demonstrated that the Apo B:Apo A-I ratio is superior to cholesterol measures and cholesterol ratios for predicting risk for myocardial infarction. In the Interheart study, comparing 12,461 myocardial infarction cases to 14,637 age and gender matched controls in 52 countries, the Apo B:Apo A-I ratio was vastly superior to any of the cholesterol parameters measured including the LDL cholesterol: HDL cholesterol ratio and the total cholesterol to HDL cholesterol ratio in all ethnic groups, in both sexes, and at all ages.
Decreasing the Apo B:Apo A-I ratio can be achieved by lowering Apo B and/or by increasing Apo A-I.
Goal – < 0.6
What to do to improve it – focus on the ‘Health Trinity’ as primary intervention. Niacin and fibrin acids have also been demonstrated to increase ApoA1.
Lp(a) Mass
This is an LDL particle containing an abnormal protein. It is an inherited abnormality and elevated levels are associated with an increased risk of developing coronary artery disease. Its structure is similar to plasminogen and it competes with plasminogen for receptor sites which causes reduced fibrinolysis and increased hypercoagulability.
Goal – < 30 mg/dL
What to do to improve it –
Lp(a) Cholesterol
When Lp(a) mass is > 30 mg/dL we reflexively measure the Lp(a) cholesterol. This helps eliminate false positives that result from the Lp(a) mass immunoassay. Such false positives are due to over-estimation of large species with high numbers of kringle repeats. Lp(a) elevation suggests a 3-5x increased risk of CVD.
Goal – < 2 mg/dL
What to do to improve it – Niacin, lifestyle
ApoB –
High LDL particle and/or low HDL is a risk factor for heart attacks and strokes. Treatment (according to the ATP III guidelines) is geared toward lowering LDL first and then focusing on TGs and HDL (generally).
However, the goal of therapy should be to decrease cardiovascular disease risk in general. People don’t have heart attacks because they have a Lipitor deficiency! They have heart attacks due to the effects of their lifestyle coupled with their genetics.
The best thing you can do to decrease your risk of cardiovascular disease is NOT to take a medicine! The best thing you can do is optimize your health through the ‘Healthy Trinity’ (nutrition, exercise, and rest).
__________________________________________________________________________
Here are some videos about the possibility that cholesterol does NOT cause heart disease.
Treatment
As I’ve said a million times:
The first treatment is to optimize your health through the ‘Healthy Trinity’
You can take medicines all day long but unless you attempt to improve your HEALTH then you are just taking a bunch of pills!
I used to subscribe to the NCEP Guidelines for the evaluation and management of cholesterol but not any longer. The evidence supporting these guidelines is entirely substandard!
Saturated fat has caused this problem. My grandparents ate loads of saturated fat and lived a long life. I don’t believe that people have ‘elevated cholesterol’ because they have a deficiency of soluble fiber, plant stanols/sterols, medications (statins), or eat too much cholesterol. There may be an improvement in lipid panels if you implement the ‘TLC diet’ as below but it is not addressing the real problem.
The real problem is the inappropriate intake of low-quality, calorie dense foods, lack of exercise, inadequate rest, and elevated stress.
The best diet is a ‘Hunter-Gatherer’ diet composed of lean meats, fruits, and vegetables and limiting sources of carbohydrates.
We cannot be healthy without addressing these issues!
_________________________________________________________________________
ATP III Therapeutic Lifestyle Changes
Here are the ‘Therapeutic Lifestyle Changes (TLCs)’ for your information. They are not a bad idea but I do not believe that implementing the TLCs alone is going to improve your health and decrease your cardiovascular disease risks.
TLC Diet
- Saturated fat <7% of total calories per day. For the average 2000 kcal/day diet that would be a total of 140 kcal of saturated fat or 15 grams of saturated fat. Make sure you know how to read the nutrition labels – they will all indicate the amount of saturated fat per serving – and total it for the entire day
- Total daily cholesterol intake <200 mg per day
- Soluble fiber intake of 10-25 grams per day. You want SOLUBLE fiber, not insoluble fiber. Insoluble fiber is the stuff in metamucil, salads, etc. Good sources of soluble fiber are found in:
- oats, oat cereals – this is why Cheerios gets the healthy label
- fruits – apples, pears, citrus fruits, berries, apricots, prunes
- vegetables – carrots, cabbage, brussel sprouts, sweet potatoes
- beans, legumes, lentils, chickpeas, and peas
- Plant Stanols & Sterols – shoot for 2 grams per day. These work by blocking cholesterol absorption in the gut. They are generally available as a supplement from most vitamin and health food stores.
Weight Management – the goal is to get a Body Mass Index (BMI) of less than 25
Increased physical activity: all exercise and activity is good. However, the ‘magic number’ that has been studied is 17 miles per week of running, jogging, or walking. Ideally, you will want to get at least 20-30 minutes of aerobic exercise on most, if not all, days of the week.
Medications
I have never seen anyone, not a single patient, not decrease their risk of cardiovascular disease when they optimally addressed their health through the ‘Healthy Trinity’. On the other hand, nobody decreases their risks by not doing anything.
For those that are not convinced, or too lazy, medications may be an option. At the same time, keep in mind that I believe that all medications are controlled poisons! They all have side effects. Additionally, many of these medications have not been proven to be beneficial.
With all of that being said, here is the information on medications for cholesterol
There are currently 4 classes of medications for the treatment of lipids. Each class has its own set of benefits and challenges.
- Statins – They tend to reduce LDL as well as TGs and improve HDL. They stabilize plaques and are anti-inflammatory. They do appear to be beneficial but they are associated with a number of risks. Read here for more information.
- Bile Acid Sequestrants – essentially bind cholesterol in the gut and it is eliminated in the stool. Examples include cholestyramine, colestipol, & colesevelam.
- Fibric Acids: typically used to reduce TGs.
- Gemfibrozil – this one has a high risk of rhabdomyolysis when combined with a statin and, therefore, they should not be used together.
- fenofibrate – this medicine is safe when used with statins.
- clofibrate.
Nicotinic Acid (Niacin) – has one of the best track records for improving HDL (10-30% improvement), which is often hard to do. Many people have difficulty with the side effects: flushing (lasts 20-30min typically), itching, and rashes. This typically resolves after a couple of weeks. This can be minimized with taking aspirin 30-60min prior to taking the niacin. Applesauce has been a ‘miracle food’ to reduce, if not eliminate, the side effects associated with Niacin. You should start with a very low dose (100mg) and increase 100mg every 4 days until you reach around 1500mg. Revolution Niacin is a controlled release Niacin and is available in our clinic.
How to improve your HDL
This can be VERY difficult to change! HDL is often genetically determined and it is hard to change it. Here are some things that can be done:
- Exercise – at least 17 miles per week (running, jogging, or walking) has a 5% increase in HDL
- Alcohol – 1-2 glasses per day (or 1 glass per day for women) has a 12% increase in HDL
- Stop tobacco use (if you are using it) – 10 % increase
- Niacin (see above) – 10-30% increase
- Weight loss if your BMI is greater than 25. If your BMI is less than 25 then losing more weight will have no additional, direct effect.
- Remove Trans-Fatty Acids from your diet
- Add Omega-3 fatty acids to your diet
- Add soluble fiber to your diet
- RevChol – 43% improvement in HDL. This supplement outperforms every other medication and supplement
______________________________________________________________________________________
More, In-Depth Cholesterol Information
There are 5 major classes of lipoproteins. Based on size (largest to smallest) they are:
- Chylomicrons
- Very Low Density Lipoprotein (VLDL)
- Intermediate Denstiy Lipoproteins (IDL)
- Low Density Lipoproteins (LDL)
- High Density Lipoprotein (HDL)
Chylomicrons:
These are lipoprotein particles that consist of triglycerides (85-92%), phospholipids (6-12%), cholesterol (1-3%) and proteins (1-2%). They transport dietary lipids from the intestines to other locations in the body. These lipoproteins enable lipids, fat, and cholesterol to be transported in the blood (fats don’t mix well with water).
Chylomicrons pick up dietary cholesterol & triglycerides from the intestine and transport them to the tissues. As they circulate they exchange products with HDL (HDL donates an Apolipoprotein C-II (APOC2) and an Apolipoprotein E) and become ‘mature chylomicrons’. An enzyme, lipoprotein lipase, removes the triglycerides from chylomicrons. Once the TGs have been distributed, the mature chylomicrons are called chylomicron remnants.
Very Low Density Lipoproteins (VLDL):
VLDL is assembled in the liver from TGs, cholesterol, and apolipoproteins. VLDL contains Apolipoprotein B100, Apolipoprotein C-I, Apolipoprotein E, Cholesterol, Cholesteryl Esters, and TGs. VLDL takes Apolipoprotein C-II and E (in the same manner as chylomicrons). Chylomicrons and VLDL are similar but chylomicrons transport exogenous products (things ingested) and VLDL transports endogenous products (things produced in the body).
VLDL transports TGs and cholesterol to the tissues. Lipoprotein lipase is the enzyme that removes the lipids from the VLDL. Once the TGs are deposited in the tissues, the VLDL becomes…
Intermediate Density Lipoproteins (IDL):
IDL is the product of removed TGs from VLDL. IDL has lost most of its TG but it retains cholesteryl esters. It also retains ApoB100 and ApoE. The ApoE has a very high affinity for the LDL receptor. When the IDL is converted to LDL it loses its ApoE.
Low-Density Lipoprotein (LDL):
LDL is generally referred to as “bad cholesterol” because LDL, when elevated, increases risk of cardiovascular disease and health problems.
Each particle of LDL contains 1 molecule of Apolipoprotein B100 and has a highly-hydrophobic core consisting of polyunsaturated fatty acid known (linoleate) and about 1500 esterified cholesterol molecules.
LDL comes in multiple particle sizes. The smaller & more dense LDL, known as pattern B, are associated with increased risk of cardiovascular disease because they can more easily penetrate the endothelium. There is good evidence that elevations of these smaller, more dense LDL particles are more closely associated with cardiovascular disease than a standard measurement of total LDL. However, it is more expensive (and less available) to measure these particles so it is not routinely performed by most physicians.
There are several that will more accurately measure cholesterol & LDL:
- Nuclear Magnetic Resonance (NMR)
- Vertical Auto Profile (VAP)
- Gel Electrophoresis
We us NMR performed through Health Diagnostics Laboratory and offer it to my patients in my clinic. It is covered by Medicare and most other insurances. If you have any kind of health insurance this test will not cost you anything! The lab does not send bills to patients no matter what your insurance actually pays. Not bad for such wonderful information! Additionally, this lab measures LDL directly so it is not impacted by food so you don’t have to be fasting for an accurate measurement of your lipids.
LDL is formed when VLDL particles release their TGs by the action of Lipoprotein Lipase. LDL particles increase the risk for cardiovascular disease as they invade the arterial endothelium & get oxidized. A complex set of biochemical reactions, stimulated by necrotic cell debris & free radicals in the endothelium, regulates the oxidation of LDL particles.
The liver is able to synthesize cholesterol via the Mevalonic Acid Pathway. The rate limiting step in this pathway is 3-hydroxy-3-methylglutaryl coenzyme A reductase (HMG CoA Reductase). This enzyme is inhibited by the Statin medications. HMG CoA Reductase activity is increased by insulin and decreased by glucagon adding to the multiple problems of excess insulin.
LDL is not directly measured by the Standard Lipid Panel but calculated by the Friedwald equation:
HDL = TC – LDL – TG(0.20)
A reduction of small, dense LDL particle is essential for decreasing the risk of cardiovascular disease and atherosclerosis. The target LDL for treatment varies based on the overall risk of cardiovascular disease for the patient. The goal with any therapy is to decrease the risk of cardiovascular disease.
Modern, western medicine uses ‘target goal’ levels because they are using medications to achieve effect. Since medicines are ‘controlled poisons’ there are side effects and risks associated with their use. We treat to a target goal simply to limit the cost of therapy and minimize risks and side effects.
High Density Lipoproteins (HDL):
These particles are referred to as high-density due to the amount of cholesterol relative to protein. HDL particles contain Apolipoprotein A1 and A2. HDL transports cholesterol from other lipoproteins and tissues back to the liver and to ‘steroidogenic organs’. The steroidogenic organs need cholesterol for the production of steroids and other hormones. The process of HDL picking up cholesterol from the tissues and taking it back to the liver is termed Reverse Cholesterol Transport (RCT).
HDL helps prevent cardiovascular disease due to its ability to pick-up cholesterol and inhibit inflammation, oxidation, activation of the endothelium, coagulation, and platelet aggregation. These factors contribute to the protective effects of HDL and why low HDL levels increase risk of CVD. In fact, you decrease your risk of death 6% & cardiovascular events 3% for every 1 mg/dl you increase your HDL.
References:
- http://circ.ahajournals.org/content/110/17/2678.full
- http://www.medpedia.com/news_analysis/68-The-Heart-Scan-Blog/entries/37255-Carbohydrate-LDL-double-whammy
- http://www.ajcn.org/content/76/2/351.short
- http://www.holistichearthealth.com/library/pdf/oats203.pdf
- http://www.trackyourplaque.com/blog/2011/03/90-small-ldl-good-news-bad-news.html
- http://www.trackyourplaque.com/blog/2009/04/blast-small-ldl-to-oblivion.html
- http://hearthawk.blogspot.com/2011/09/franken-wheat-my-own-mad-genetic.html
- http://www.nhlbi.nih.gov/guidelines/cholesterol/atp3xsum.pdf
- http://chriskresser.com/cholesterol-doesnt-cause-heart-disease
- http://jama.ama-assn.org/content/272/17/1335.abstract
- http://www.ncbi.nlm.nih.gov/pubmed/1355411
- http://www.spacedoc.com/
- https://www.codemap.com/atherotech/index.cfm?d=OKLAHOMA&state=04302